Dermatomyositis : Navigating Causes, Symptoms, and Treatment Strategies
Dermatomyositis, a rare autoimmune disease, affects muscles and skin, leading to muscle inflammation and skin rash. The condition, believed to be caused by a mix of genetic and environmental factors, requires ongoing medical care for management.
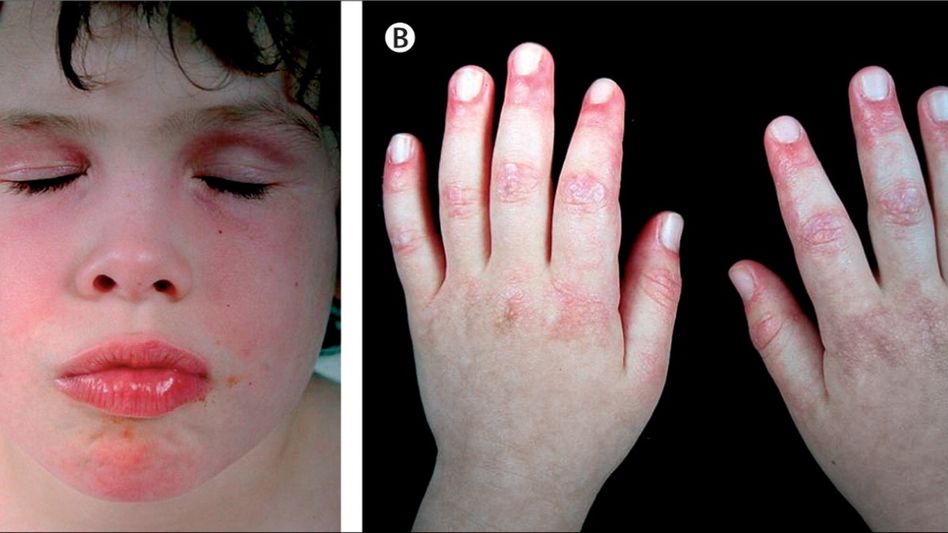
Dermatomyositis is a rare autoimmune disease that primarily affects the muscles and skin. It is characterized by inflammation of the muscles (myositis) and skin rash. This condition can impact various body systems and may involve other organs. The exact cause of dermatomyositis is not well understood, but it is believed to involve a combination of genetic and environmental factors.
Common symptoms of dermatomyositis include muscle weakness, especially in the hips, thighs, shoulders, and neck, along with a distinctive skin rash. The rash often appears on the face, eyelids, knuckles, elbows, knees, chest, and back. Individuals with dermatomyositis may also experience fatigue, difficulty swallowing, and joint pain.
Diagnosis typically involves a combination of clinical evaluation, blood tests, imaging studies, and sometimes a muscle biopsy. Treatment aims to manage symptoms and may involve the use of corticosteroids to reduce inflammation, immunosuppressant drugs, and physical therapy to maintain muscle strength and flexibility.
Since dermatomyositis is a chronic condition, ongoing medical care and monitoring are essential to adjust treatment and address any emerging symptoms or complications. While there is no cure, proper management can help improve the quality of life for individuals with dermatomyositis.
Understanding the Roots: Causes of Dermatomyositis
The exact cause of dermatomyositis remains elusive, making it a challenging condition to decipher. However, it is widely accepted that this autoimmune disease involves a complex interplay of genetic and environmental factors. The immune system, designed to protect the body, mistakenly targets its tissues, leading to inflammation in the muscles and skin.
Genetic predisposition may play a role, as certain individuals may be more susceptible to autoimmune conditions like dermatomyositis due to their genetic makeup. Environmental triggers, such as infections or exposure to certain medications, could potentially set off the immune system's aberrant response.
Unveiling the Manifestations: Symptoms of Dermatomyositis
Dermatomyositis manifests through a spectrum of symptoms, impacting both the muscular and dermatological systems. Recognizing these symptoms is crucial for early diagnosis and effective management:
-
Muscle Weakness: One of the hallmark symptoms is progressive muscle weakness, particularly in the proximal muscles (those closest to the trunk), such as those in the hips, thighs, shoulders, and neck. This can result in difficulties with everyday activities like climbing stairs or lifting objects.
-
Skin Rash: A distinctive skin rash is a common feature of dermatomyositis, often taking the form of a violet or reddish rash. It frequently appears on the face, eyelids, knuckles, elbows, knees, chest, and back. This rash, known as a heliotrope rash, is a key diagnostic indicator.
-
Fatigue: Individuals with dermatomyositis often experience persistent fatigue, which can significantly impact their daily lives. The combination of muscle weakness and immune system activation contributes to this overwhelming tiredness.
-
Difficulty Swallowing: Dermatomyositis can affect the muscles involved in swallowing, leading to dysphagia (difficulty swallowing). This can result in complications and necessitate dietary modifications.
-
Joint Pain: Joint pain and inflammation may accompany muscle symptoms, causing discomfort and limiting mobility.
Navigating the Maze: Diagnosis and Evaluation
Diagnosing dermatomyositis requires a multidimensional approach, often involving various medical assessments:
-
Clinical Evaluation: A thorough physical examination by a healthcare professional is crucial to identify characteristic symptoms such as muscle weakness and skin rash.
-
Blood Tests: Blood tests, including creatine kinase (CK) levels, can help assess muscle damage and inflammation. Elevated levels may indicate muscle involvement.
-
Imaging Studies: Techniques such as magnetic resonance imaging (MRI) and electromyography (EMG) may be employed to evaluate muscle function and detect abnormalities.
-
Muscle Biopsy: A muscle biopsy is often performed to examine muscle tissue microscopically, confirming inflammation and aiding in the diagnosis.
Crafting a Shield: Treatment Approaches for Dermatomyositis
While dermatomyositis has no cure, various treatment modalities aim to manage symptoms, reduce inflammation, and improve overall quality of life:
-
Corticosteroids: Prednisone, a type of corticosteroid, is frequently prescribed to suppress inflammation. However, long-term use may lead to side effects, necessitating careful monitoring.
-
Immunosuppressive Medications: Additional medications, such as methotrexate, azathioprine, or mycophenolate mofetil, may be employed to modulate the immune system and curb inflammation.
-
Topical Treatments: Skin symptoms can be addressed with topical treatments, including corticosteroid creams, to alleviate rash and discomfort.
-
Physical Therapy: Physical therapy plays a pivotal role in maintaining muscle strength and flexibility. Tailored exercises help individuals manage muscle weakness and enhance mobility.
-
Occupational Therapy: Occupational therapists assist in adapting daily activities to accommodate muscle weakness, fostering independence.
-
Sun Protection: Given the skin involvement, sun protection measures, such as sunscreen and protective clothing, are crucial to manage and prevent skin rashes.
-
Pain Management: Over-the-counter or prescription pain medications may be recommended to alleviate muscle and joint pain.
-
Regular Monitoring: Ongoing medical supervision is essential to assess treatment efficacy, manage potential side effects, and address emerging symptoms or complications.
Dermatomyositis, with its intricate blend of muscular and dermatological manifestations, underscores the challenges posed by autoimmune diseases. With advancements in medical understanding and treatment options, individuals grappling with dermatomyositis can embark on a path towards improved symptom management and enhanced quality of life. A collaborative approach between healthcare professionals, patients, and support networks is crucial in navigating the complexities of this rare autoimmune disorder. As research continues to unveil the mysteries surrounding dermatomyositis, the journey towards more effective treatments and, perhaps one day, a cure, offers hope on the horizon.
Copyright©2025 Living Media India Limited. For reprint rights: Syndications Today









